Neurofibromatosis Type 1 (NF1)
Neurofibromatosis (NF) is a group of genetic conditions that cause tumours to grow on nerves throughout the body. The main types of NF include neurofibromatosis type 1 (NF1) and schwannomatosis (SWN).
Neurofibromatosis type 1 (NF1) is the most common form of NF, affecting approximately 1 in every 2,500 births.
What Is NF1?
NF1 is a lifelong genetic condition that primarily affects the skin, nervous system, and bones. It affects people of all genders, races, and ethnicities.
Although NF1 is present at birth, it is most often diagnosed in childhood. Some signs appear early, while others develop gradually over time, which can delay diagnosis. Because NF1 can look different from one person to another, early features are sometimes missed, particularly by healthcare providers who are less familiar with the condition.
How Does NF1 Affect People?
NF1 affects people very differently even within the same family.
Some individuals have mild features that require little medical intervention, while others experience more complex health challenges. It is not possible to predict how NF1 will affect any one person.
Most people with NF1 have mild features and live full, productive lives with appropriate monitoring and care.
Common Signs and Features
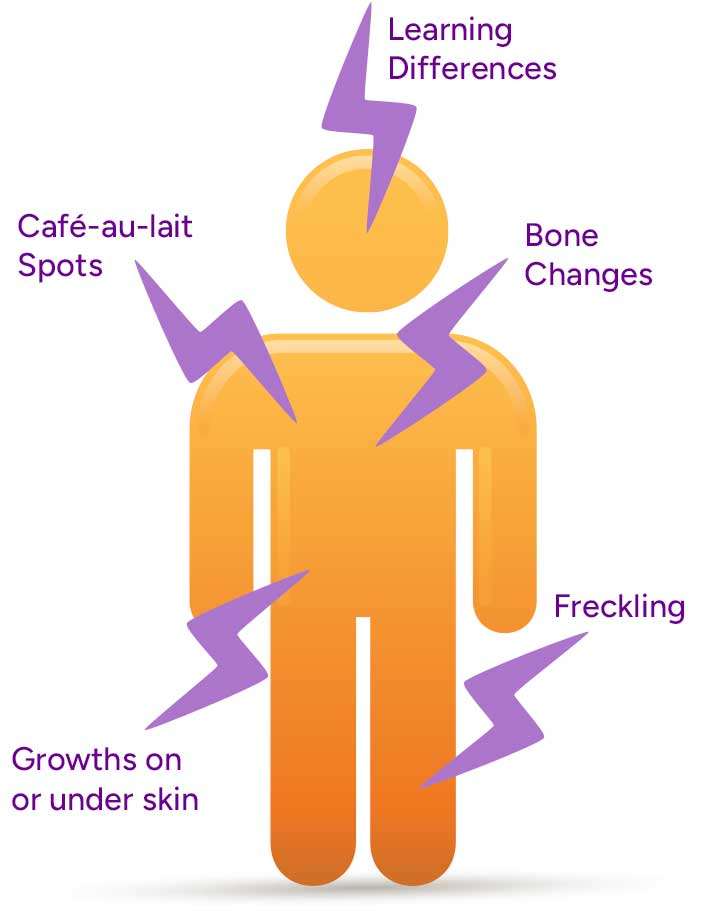
NF1 may affect the skin, nerves, bones, eyes, and learning. Common features may include:
- Café-au-lait spots (light brown skin patches)
- Freckling in areas such as the armpits or groin
- Neurofibromas, which are benign (non-cancerous) growths on or under the skin
- Learning differences, which affect about half of people with NF1
- Bone changes, such as scoliosis (curvature of the spine)
Not everyone will experience all of these features.
How Is NF1 Diagnosed?
Only a physician can make a formal diagnosis of neurofibromatosis type 1 (NF1). Diagnosis is usually based on a combination of:
- Physical features
- Medical and family history
- Eye examinations
- Imaging or other tests, when needed
Because features of NF1 can emerge slowly and vary widely, diagnosis may not happen right away even though the condition is present from birth.
Diagnostic Criteria
The diagnostic criteria for NF1 were updated in 2021. To make a diagnosis, an individual must meet two or more of the following criteria:
- Six or more café-au-lait macules (light brown skin spots)*
- Freckling in the armpits (axilla) or groin*
- Two or more neurofibromas of any type, or one plexiform neurofibroma
- Two or more Lisch nodules (benign spots in the iris of the eye)
- An optic pathway glioma
- A distinctive bone lesion (such as sphenoid dysplasia or tibial dysplasia/pseudarthrosis)
- A pathogenic NF1 variant identified through genetic testing
- A parent with NF1 based on the above criteria
*At least one of the pigmentary features must be present on both sides of the body.
If you have questions about diagnosis, we encourage you to speak with your healthcare provider. We can also help you understand what questions to ask.
Tumours and Cancer Risk
Most tumours associated with NF1 are benign (non-cancerous) and often do not require treatment.
In some situations, tumours may cause concerns if they press on nearby nerves or tissues. A small percentage of people with NF1 develop malignant (cancerous) tumours, but most people with NF1 will never develop cancer.
Some health risks are higher in people with NF1. For example, women with NF1 have an increased risk of breast cancer and may require earlier or more frequent screening than the general population.
Your healthcare provider can help determine appropriate screening based on your individual situation. We also offer educational resources to support informed advocacy and care.
Genetic Testing for NF1
Genetic testing for NF1 is available, but it is a personal choice and not required for everyone.
In British Columbia, genetic testing for NF1 is typically accessed through the Provincial Medical Genetics Program. A referral can be made by a primary care provider or specialist.
NF1 can often be diagnosed clinically, based on established criteria, without genetic testing. Because features may appear gradually, a clinical diagnosis may be made before testing is considered.
People choose genetic testing for a variety of reasons, including:
- Confirming a diagnosis
- Supporting diagnosis in young children
- Understanding inheritance and family planning options
Genetic testing cannot predict severity or specific complications, and results may take time. Public testing is not a rapid service, and wait times can vary. Some individuals choose private genetic testing to obtain results more quickly. This is a personal decision and may involve out-of-pocket costs.
A genetics healthcare provider or genetic counsellor can help individuals and families decide what feels right for them.
Are There Treatments for NF1?
There is currently no cure for NF1, but many symptoms and complications can be managed. Care may include:
- Regular monitoring and follow-up
- Surgery for tumours that cause pain, functional problems, or other concerns
- Medications or therapies to manage specific symptoms
- New and emerging treatments for certain NF1-related tumours
Not all neurofibromas need to be treated or removed. Treatment decisions are individualized and guided by healthcare providers familiar with NF1.
Living With NF1
NF1 is a lifelong condition, but support makes a meaningful difference.
Care is often coordinated by a family doctor, with referrals to specialists as needed. Because British Columbia does not yet have a dedicated multidisciplinary NF clinic, navigating care can sometimes feel challenging.
We can help.

Support in British Columbia
The Tumour Foundation of BC offers:
- One-to-one support
- Help understanding diagnosis and care options
- Guidance navigating the healthcare system
- Educational resources and community connection
You don’t have to navigate NF1 alone.
